Ways4eu WordPress.com Blog
SPA View of ways4eu.wordpress.com
🩺 The Quiet Drama of Coeliac Disease: Gluten, Gut, and an Unassuming Superpower
By Kinda Cool
on Wed Apr 15 2026
🩺 A Quiet Medical Thriller
On April 15, 2026, the internet did what it does best: it turned a quiet medical condition into a story you didn’t know you needed to hear today. Our featured subject, modest in magnitude but mighty in impact, is coeliac disease. If you’ve ever wondered how gluten can transform a simple bite into a plot twist inside your own small intestine, you’re in the right place.
🧬 The Plot Synopsis
First, a quick plot synopsis: coeliac disease is a chronic autoimmune condition that targets the small intestine when gluten—those wheat, barley, and rye proteins—crashes the party. For people with a genetic predisposition, gluten triggers inflammation that damages the lining of the gut, which in turn can sap the body’s ability to absorb nutrients. It sounds like a medical thriller, and in many ways, it is—the stakes are health, energy, and, yes, avocado toast futures.
🔍 The Famous Paradox of Symptoms
Here’s the funny paradox that never fails to amuse: the symptoms can be famously unglamorous. Some people show classic signs like chronic diarrhea, weight loss, and abdominal pain. Others experience a sweep of non-classic symptoms—anemia, osteoporosis, skin rashes, or even neurological issues. Bodies don’t always wear their secrets on their sleeves.
🔬 The Diagnostic Journey
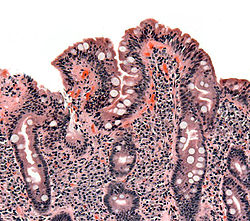
Diagnosis is a careful, multi-layered affair. It often starts with blood tests that look for specific antibodies and then may proceed to a biopsy of the small intestine. The biopsy is the character moment: it confirms whether the mucosal lining has the telltale signs of damage.
🍽️ Strict, Not Glamorous, But Heroic
Treatment, in a word, is lifestyle: a strict gluten-free diet. And by strict, we mean strict. Even tiny traces can provoke symptoms and slow healing, so vigilance becomes a daily habit, not a seasonal reset. The good news is bright: many patients see symptom improvement within days of eliminating gluten, and long-term risks can be substantially mitigated when the gut has room to repair.
🌎 Why It Matters to Everyone
Why does this matter to the broader world, beyond the gluten-free aisle at the grocery store? Awareness matters. Diagnoses of coeliac disease have risen—partly because we’re better at recognizing it, partly because blood tests are more accessible, and partly because people feel empowered to ask questions about their own bodies. Yet many cases still go undiagnosed, which makes early detection not just a personal win but a public health win.
🍳 The Kitchen as Battlefield and Laboratory
Gluten-free cooking has evolved from a niche hobby into a culinary subculture with real science behind it. It’s not merely a lifestyle trend; it’s a response to a biological reality for those who live with coeliac disease. The kitchen becomes both battlefield and laboratory: you learn which flours behave, how to bind without gluten’s gluteny glue, and why cross-contamination can feel like an existential threat.
📋 Practical Signs to Watch For
If you’re reading this and wondering how to tell whether you or a loved one might be affected, here are a few practical signs—though only a medical professional can diagnose: Persistent gastrointestinal symptoms after consuming gluten; unexplained iron-deficiency anemia or short stature in children; ongoing fatigue, bone or joint pain, rashes without an obvious cause; or a family history of autoimmune conditions.
✨ A New Dawn After Diagnosis
In the end, coeliac disease isn’t a villain to fear; it’s a signal—an opportunity to listen to the body more closely, to question assumptions, and to celebrate the resilience that comes from adapting with intellect and humor. If a tiny gluten molecule can catalyze such a chain reaction, imagine what you’re capable of when you tune in, learn, and choose your gluten with intention.
Wikipedia Featured Article — read the full article: Wikipedia© H.J. Sablotny — All rights reserved. The texts on this blog are the intellectual property of H.J. Sablotny.Images are subject to their respective copyright holders and are used for illustration purposes only.